Agentic claims processing for P&C carriers
Lawyers have AI.
Insurers have ClaimBuddy.
A second pair of eyes for every BI examiner. ClaimBuddy reviews demand letters and medical packets in minutes, flags missed items with citations to the source page, and helps your team settle claims with sharper data.
Built with senior BI examiners at top-tier US auto carriers.
Car insurance loss ratios are under pressure.
rise in car insurance prices since 2010, far outpacing inflation.
of carrier loss ratios driven by personal injury claims.
of PI claims projected to involve attorney representation by 2030, up from 35% in 2010.
Plaintiff law firms have driven the cost to file a personal injury claim from $2,000+ down to under $100 with agentic workflows. Demand letters are longer, more frequent, and increasingly machine-drafted. Some packets exceed 10,000 pages. Examiners are expected to read every page. The math no longer works without help.
"We get medical records sometimes from attorneys that are 10,000 pages. And an examiner is going to have to go through every single page."
"We've talked to a lot of vendors… they are missing a whole lot of stuff."
A safety net for every claim.
Catches what gets missed.
ClaimBuddy reviews the examiner's evaluation against thousands of pages of medical evidence. Flags treatment gaps, prior injuries, billing inconsistencies, and unsupported procedures. Every flag links to the source page.
Speeds up the cycle.
Demand and medicals are processed in parallel with the examiner. The cross-check completes in 5 to 15 minutes after evaluation. No new wait time.
Sharpens the negotiation.
Surfaces historic attorney behavior, firm settlement patterns, and a strengths and weaknesses view of the case. Examiners walk in prepared.
The product
Safety net first. Negotiation prep as add-on.
Catches what gets missed before settlement.
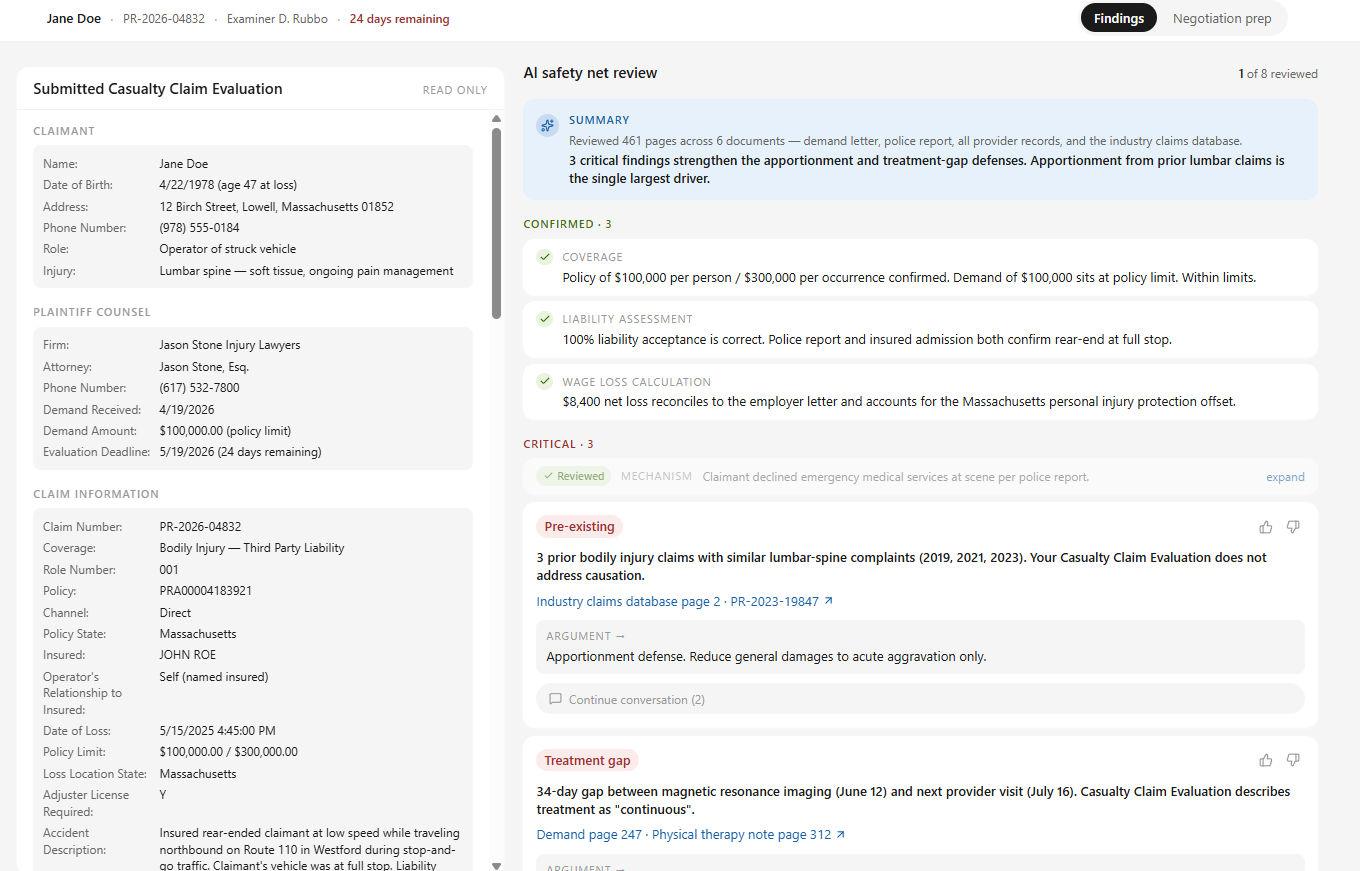
ClaimBuddy reads the full demand, the medical packet, and the examiner's Casualty Claim Evaluation side by side. Confirmed items are marked. Critical findings — pre-existing conditions, treatment gaps, billing inconsistencies — surface as cards with the source page one click away.
- Confirms coverage, liability, and wage-loss math first.
- Flags critical findings with a one-click jump to the source page.
- Examiner can accept, push back, or open a chat against any flag.
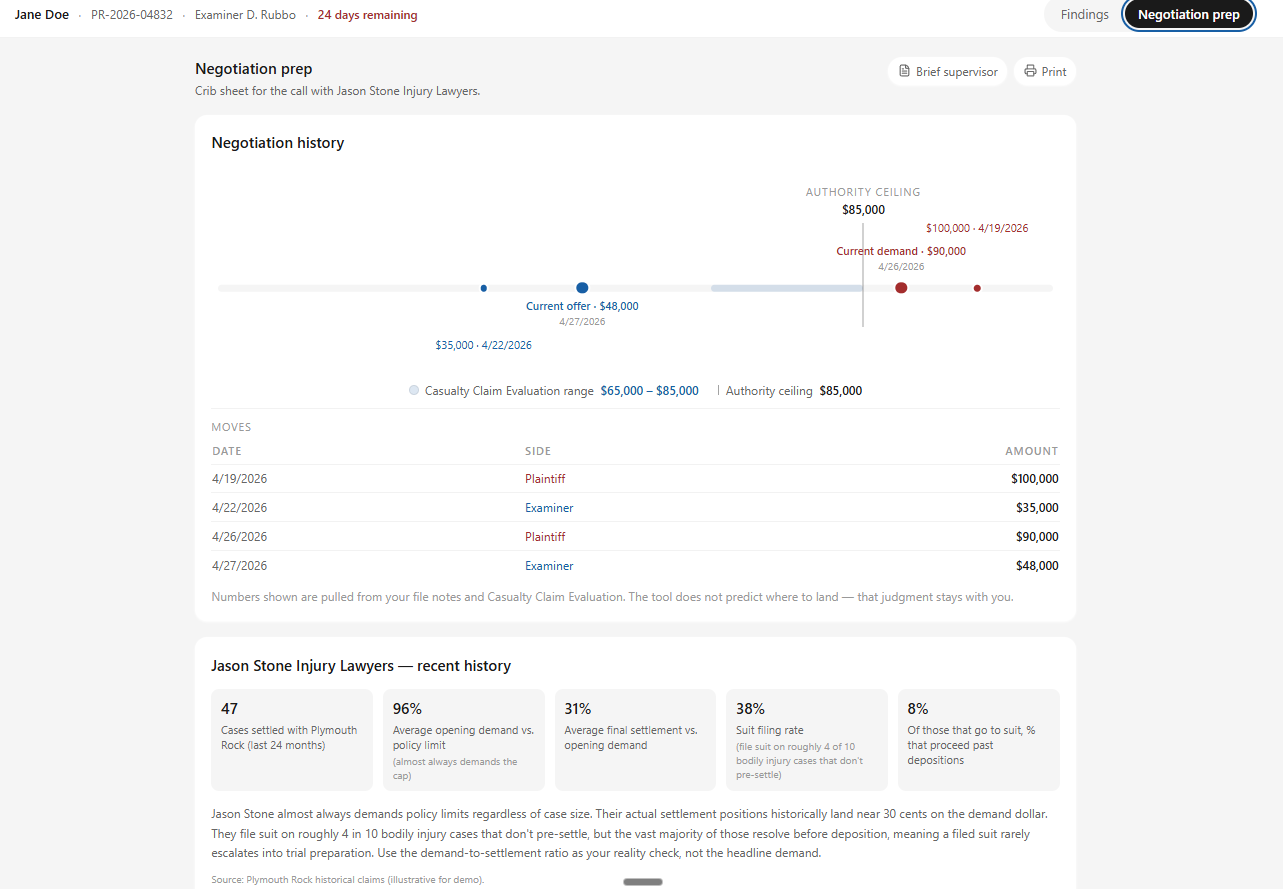
A crib sheet for the call, grounded in real data.
Plots every move on the file against the evaluation range and authority ceiling. Pulls historic settlement behavior on the opposing firm — opening demand vs. final settlement, suit-filing rate, proceed-past-deposition rate — so the examiner walks in with a reality check, not a headline demand.
- Negotiation history charted against your evaluation range and authority.
- Firm-level history: opening demand vs. final settlement, suit-filing behavior.
- Print a one-page brief for supervisor sign-off before the call.
"This is exactly how I would design the process if I was building software."
Parallel work, then a quick cross-check.
- Step 1Demand letter received
- Step 2Read records and build evaluation
- Step 3Set valuation range
- Step 4Cross-check with ClaimBuddy
- Step 5Send to attorney
- Step 1Ingest demand and medicals
- Step 2Extract facts and run checks
- Step 3Build evidence index
- Step 4Surface flags with sources
Parallel, not blocking. The examiner never waits on the tool.
Examiner stays the decider. Flags are advisory and can be accepted, refuted, or probed.
Sourced to the document. Every flag links to the page in the medical packet. No black-box judgments.
Built for the work BI teams actually do.
Medical chronology in minutes.
Reduce 1,000+ page packets to a sourced timeline with treatment, diagnoses, and gaps.
Pre-existing condition detection.
Cross-checks against industry claim databases to surface prior injuries that affect apportionment.
Treatment validity and billing review.
Flags procedures that lack medical necessity or fall outside Medicare and state fee schedules.
Negotiation prep.
Pulls historic settlement behavior on the opposing firm and attorney. Builds a fact-based view going into the call.
Potential savings
What 1%, 3%, and 5% would mean on a $300M BI book.
A senior BI examiner estimates ClaimBuddy would surface missed information in roughly two-thirds of cases above the $25K examiner-authority threshold. A 1% to 5% improvement on a typical mid-sized auto book translates into $3M to $15M in annual savings.
~$200 per claim · ~$50K per examiner
~$600 per claim · ~$150K per examiner
~$1,000 per claim · ~$250K per examiner
Illustrative model based on a ~60-examiner book, ~15,000 cases per year, and an average claim value of $20K to $30K. Per-claim and per-examiner figures are book-level averages. A pilot benchmarks the assumption against your own outcomes.
Defense-side. AI-native. Built with examiners.
Defense-side by design.
Most AI in personal injury is built for plaintiff firms. ClaimBuddy is the only AI-native platform built for the carrier. We exist to level the playing field.
Built with examiners, not for them.
Co-designed with senior BI examiners at multiple top-tier carriers. Iterated with claims leadership. Every feature has a real user behind it.
No reliance on AI output.
ClaimBuddy never predicts a settlement number. It surfaces facts and flags the examiner can verify in one click. Examiner judgment stays the authority.
Pilot proposal
One month to set up. Two months to prove it.
Setup
Connect to closed BI claims. Calibrate the safety net to your evaluation format, fee schedules, and authority thresholds. Train two to three lead examiners.
Run
ClaimBuddy reviews live or recently-closed claims in parallel with examiners. Weekly readouts on flags surfaced, accepted, and dismissed.
Benchmark
Compare findings against the team's own outcomes. Quantify saved indemnity, time saved per file, and accuracy of flags. Decide rollout scope.
A team that has built AI agents on both sides of the claim.
Second-time founder. Previously built AI agents for personal injury law firms, giving ClaimBuddy direct visibility into how the plaintiff side uses automation. Background: Harvard Business School (MBA 2026), Boston Consulting Group, Jain Global, OWheels.
Machine learning engineer. Previously built AI agents for insurance brokerages. Background: MIT, US Air Force, US Air Force Academy.
Built for the security review.
SOC 2 Type II in progress.
Audit underway with a Big Four firm. Report available under NDA.
HIPAA-aligned data handling.
PHI handled under signed BAAs. Encrypted at rest with AES-256 and in transit with TLS 1.3.
US data residency.
All processing on AWS US-East and US-West regions. No customer data leaves the United States.
No model training on customer data.
Carrier data is never used to train foundation models. Each customer gets an isolated tenant.
Common questions from claims executives.
Ready to give your examiners a working safety net?
Pilots start at one month of setup and two months of running on closed claims. We benchmark against your team's own outcomes.